In this article
The male sex hormone – testosterone (T) declines gradually after the age of 30. However, low T levels are only one of the signs that you may need treatment.

Keep in mind that your symptoms may also be caused by other hormonal deficiencies, thyroid problems, depression, or various substances.
Thus, you should always visit an experienced medical doctor who will diagnose you and decide the best course of therapy for your condition.
How low testosterone levels affect men
Low testosterone levels (hypogonadism) can lead to negative consequences for multiple organs and systems.
Without T’s anabolic effects, your body can no longer maintain optimal muscle and bone strength, hemoglobin levels, or sperm production.
Furthermore, some of the long-term negative effects of hypogonadism may include dangerous medical complications.
The American Urological Association recommends that all clinicians inform their patients that low T carries a risk for potentially fatal conditions such as heart disease.
Besides, low T may be a sign of a serious underlying disorder that affects the hypothalamus, pituitary gland, or testes
For example, tumors or inflammatory conditions such as sarcoidosis can affect the pituitary and lead to secondary hypogonadism.
Infections such as HIV/AIDS and tuberculosis can also damage the gland and result in low T. Systemic diseases that can lead to a decrease in testosterone are chronic liver and kidney disease.
Other risk factors that can lead to low T include:
- Testicular injury or infection
- Head trauma or surgery
- Exposure to radiation
- Alcohol abuse
- Opioid or corticosteroid therapy
- Obesity and type 2 diabetes
- Aging
Recognizing the signs of low T and performing a thorough examination is the key to determine the exact cause.
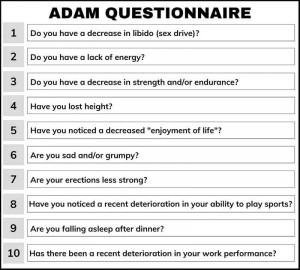
One of the novel methods that can help detect the symptoms of low T is the quantitative questionnaire called ADAM (Androgen Deficiency in the Aging Male).
Studies reveal that ADAM correlates well to the results of other questionnaires as well as the serum testosterone levels of the tested subjects. It is a 10-question test that investigates whether the patient has signs of low T.
If you answered “yes” to questions 1 or 7, or answered “yes” to more than 3 questions, you may have low testosterone levels. Talk to your doctor and get the appropriate tests done to confirm the presence of the disease.
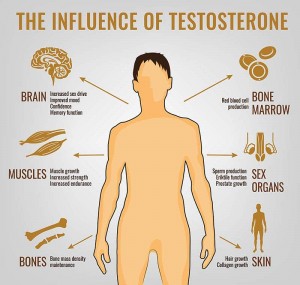
How testosterone affects men’s health
Testosterone is the hormone of masculinity. Its production is at its highest during puberty while the male sexual characteristics fully develop.
Trials have revealed that the age-related decline is more noticeable in the morning T levels when its production should be the highest. Thus, testosterone appears to lose its circadian rhythm with aging.
However, studies reveal that the average levels of T in most men aged 40-80 remain in the range of 450-500 ng/dL. The value considered as low testosterone in men, regardless of age, is 300 ng/dL, measured in the morning.
Common symptoms of testosterone deficiency in men
The only way to know if you have low T is to visit a medical specialist such as an endocrinologist.
Your doctor will determine whether you have any symptoms of low testosterone and assign tests if needed. The most common complaints in patients with hypogonadism include:
- decreased libido and erection problems
- lack of energy
- memory impairment
- mood swings
- loss of pubic and axillary hair
- decreased endurance and work performance
- falling asleep right after dinner
You may also notice body composition changes such as loss of muscle mass and extra weight gain
Some of these symptoms might be age-related or caused by other health problems. Thus, only visiting an endocrinologist and testing your testosterone levels can confirm whether or not you have hypogonadism.
What low T conditions require treatment?
All conditions which involve low T levels that lead to symptoms require therapeutic management.
The causes of low T can be categorized, depending on which part of the hypothalamic-pituitary-gonadal axis (HPG axis) is not functioning properly.
The role of the hypothalamus and the pituitary gland is to produce luteinizing hormone (LH) and follicle-stimulating hormone (FSH) which stimulate the testicles to produce T.
Problem to any component of the HPG axis can lead to low T
In some cases, the functions of both the testicles and the pituitary gland are affected.
Such is the case of late-onset hypogonadism (andropause). Evidence reports that andropause is caused by the waning of both pituitary and testicular function as age advances.
Andropause (age-related decline)
Late-onset hypogonadism is commonly called andropause or male menopause.
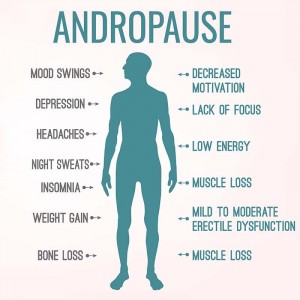
Men do not suffer from a sudden drop in testosterone unless there is an external factor such as a tumor or trauma. They experience a gradual decline in T levels by about 1-2% every year as they age.
In some males, the decline can lead to pathologically low T levels and symptoms. Thus, andropause is not something all men experience.
Late-onset hypogonadism is a medical condition that occurs in men in their 40s, 50s or older. The symptoms involve typical signs of low testosterone, such as sexual dysfunction and depression.
The comparison with female menopause might be due to the presence of common symptoms such as lack of libido, mood swings, fatigue, hot flashes, and fat gain.
However, in some cases, these signs are not related to T levels at all. Causes other than late-onset hypogonadism may include psychological problems, age-related crises, or unhealthy lifestyle choices.
Hypogonadism
Depending on whether hypogonadism is caused by problems with the hypothalamus and the pituitary gland, or a testicular disorder, it is classified as either primary or secondary.
If the pituitary gland does not stimulate the testicles to produce T, the condition is called secondary hypogonadism, and causes include:
- Congenital conditions (Kallmann syndrome)
- Damage due to tumors, brain injury, surgery, infections, infarction, or radiation
- Medications (opioids, glucocorticoids, anabolic steroids)
If the testicles can no longer function, even with proper stimulation, then the condition is called primary hypogonadism, and its usually the result of:
- Congenital disorders (Klinefelter’s syndrome)
- Anatomical problems (cryptorchidism or varicocele)
- Damage due to tumors, surgery, infections, torsion, chemotherapy, or radiation
- Testicular atrophy due to secondary hypogonadism
Unfortunately, primary and secondary hypogonadism are not reversible conditions
Low testosterone diagnosis
Your physician can diagnose you with hypogonadism only after a thorough medical examination and several tests.
In some states. your medical exam may also happen during a telehealth consultation. However, testing your testosterone levels requires visiting a certified lab in person.
A proper diagnosis requires at least two blood tests of testosterone, performed on two different days. Testosterone must be measured during the morning, usually between 7-10 AM when natural production is the highest.
If both measurements reveal that your total T levels are under 300 ng/dL, then your endocrinologist will run additional tests to determine whether you have primary or secondary hypogonadism.
If your LH and FSH are high, this indicates that you have primary hypogonadism. Normal or low LH and FSH suggest secondary hypogonadism.
Only after you have been diagnosed, you may get a testosterone prescription from your doctor and start treatment for your symptoms.
Optimal treatment for low T in men
Treatment for hypogonadism involves administering exogenous testosterone. It increases your body’s T levels back to normal values and alleviates your symptoms.

There are different methods to administer T in the body, but both patients and clinicians favor testosterone injections as the most reliable, affordable, and safe form of TRT.
Injections will help you achieve the quickest improvement in low T symptoms
If you do not have any signs or complaints related to low T levels, then TRT is not recommended. There is not enough evidence to justify testosterone use in the absence of symptoms.
What to expect from TRT?
Before starting the treatment, you should be aware that testosterone therapy can help improve all symptoms of hypogonadism except infertility.
The possible benefits of TRT include improved sexual function, better memory, enhanced body composition, and reduced symptoms of depression.
Furthermore, the therapy may lead to some unexpected advantages, such as improved heart health. One large trial involving 83 000 men reveals that achieving normal T levels with TRT reduces the risk of heart attack, stroke, and premature death.
Other studies report conflicting results of testosterone on heart health, which might be related to the use of higher, supraphysiological doses.
Unfortunately, infertility can be a side effect of TRT, due to the suppression of the natural T synthesis. If you wish to remain fertile, you should notify your doctor before starting testosterone therapy.
Other adverse effects to be aware of include acne, oily skin, high red blood cell count, and increased risk of prostate cancer.
Currently, there are no other options for the treatment of hypogonadism. The effectiveness of nutritional and herbal supplements for low T is not supported by the available scientific literature. In fact, studies report that some of the ingredients can have negative effects on natural T production.
Precautions and monitoring
Testosterone therapy is not risk-free, so make sure to warn your doctor if you have any of the following conditions:
- Prostate enlargement and problems with urination
- Family or medical history of prostate or breast cancer
- Severe obstructive sleep apnea
- History of cardiovascular disease, heart attack, or stroke
- Elevated red blood cells or platelets (thrombocytes)
Your doctor will help you minimize the risk of adverse reactions by monitoring your testosterone therapy. The process requires regular checkups which are done every 3-6 months during the first year and then annually.
During your visits, your physician will also run tests that will help evaluate your response to the treatment. If there are any negative signs or problems with TRT, an experienced endocrinologist can adjust the therapy, in order to ensure its safety and effectiveness.
The first benefits of testosterone therapy will occur after at least 3 weeks of treatment and involve improved libido, erectile function, mood, and quality of life.
After 2-3 months you may also experience an increase in muscle size, strength, and fat loss. Continuous TRT for 6 months can also increase your bone mineral density.